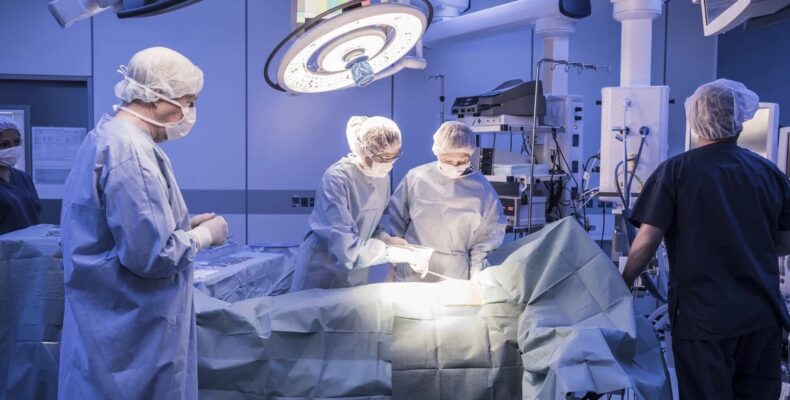
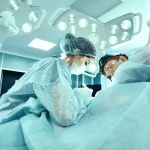
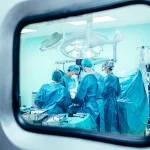
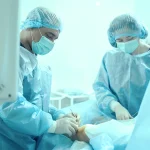
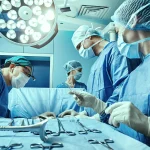
Spend enough time in complex operating rooms, whether in endovascular suites, hybrid theatres, or advanced minimally invasive surgery, and a pattern becomes clear. The visible success of a procedure is often attributed to the surgeon and the technology. What remains less visible, but no less critical, is the layer of expertise that connects the two.
That layer is the clinical specialist.
Despite their growing presence in modern operating environments, clinical specialists are still widely misunderstood, sometimes seen as technical support, sometimes as product representatives, but rarely recognized for what they actually are: operational enablers of safe, effective, and reproducible procedures.
Bridging the Gap Between Technology and Practice
The introduction of advanced medical technologies has fundamentally changed how procedures are performed. Devices are no longer passive tools; they are systems, often with complex deployment mechanics, nuanced behavior, and narrow margins for error.
No matter how skilled the operator, there is always a learning curve.
Clinical specialists exist to shorten that curve. They bring a level of device-specific familiarity that cannot be replicated through manuals or occasional training sessions. Having supported dozens—sometimes hundreds—of procedures across different centers, they develop a practical understanding of how a device behaves under real conditions, not just ideal ones.
In many cases, they are the only individuals in the room who have seen that device fail—and recover—from failure.
Consistency in High-Variability Environments
Operating rooms are dynamic environments. Anatomy varies, patient conditions evolve, and no two cases unfold in exactly the same way. In such settings, consistency becomes a challenge.
Clinical specialists contribute to consistency not by replacing clinical judgment, but by supporting it. They help standardize key aspects of the procedure—device preparation, sequencing, troubleshooting—so that variability is reduced where it can be controlled.
Over time, this translates into more predictable outcomes, shorter procedural times, and greater confidence among the team.
The First Cases: Where They Matter Most
The value of a clinical specialist becomes most evident during the early phase of adopting a new technology. The first cases are where uncertainty is highest. Even experienced operators are navigating unfamiliar workflows, device characteristics, and potential complications.
At this stage, small technical details matter. How a device is prepared, how it is introduced, how it is deployed—these are not trivial steps. They are the difference between a smooth case and a difficult one.
Clinical specialists provide real-time guidance in these moments. Not as decision-makers, but as informed partners who can anticipate challenges and offer practical solutions based on prior experience.
This early support often determines whether a program builds momentum or stalls.
Beyond the Procedure: Building Institutional Knowledge
One of the most overlooked contributions of clinical specialists is what happens outside the operating room. Their role extends into training, workflow development, and knowledge transfer across the institution.
They help educate nursing teams on instrument handling, assist biomedical staff in understanding system requirements, and support physicians in refining technique over time. In doing so, they contribute to building internal capability within the hospital.
This is where their impact becomes scalable.
A well-supported program does not remain dependent on external expertise indefinitely. Instead, it evolves—absorbing knowledge, refining processes, and developing its own internal proficiency. Clinical specialists play a key role in accelerating this transition.
The Risk of Underutilization
Despite their value, clinical specialists are not always integrated effectively. In some institutions, their involvement is limited to the initial installation or a handful of cases. In others, they are treated as optional rather than essential.
This underutilization carries consequences.
Without consistent technical support, variability increases. Minor issues take longer to resolve. Confidence within the team may erode, particularly in complex or unexpected situations. Over time, the perceived difficulty of the technology can outweigh its benefits.
What could have been a high-performing program becomes inconsistent.
A Shift in Perspective
As medical technologies continue to evolve, the operating room is becoming more interdisciplinary. Success is no longer defined by individual expertise alone, but by how well different layers of knowledge—clinical, technical, and operational—are integrated.
In this context, the role of the clinical specialist is not peripheral. It is central.
Recognizing this requires a shift in perspective. Instead of viewing them as adjunct support, institutions should consider them part of the procedural ecosystem—particularly in the early and intermediate stages of program development.
Closing Perspective
Modern procedures are more complex than ever, but they are also more structured. The difference between difficulty and mastery often lies in how well that structure is supported.
Clinical specialists bring a form of experience that is both specific and transferable. They help translate technology into practice, reduce variability, and support teams as they move from adoption to proficiency.
In many ways, they are the quiet stabilizing force in environments where precision matters most.
Their impact may not always be visible—but it is almost always felt.
Legal Disclaimer
The content provided in this article and throughout the AVISTA platform is intended for educational and informational purposes only. It does not constitute medical advice, diagnosis, or treatment, nor is it intended to replace the clinical judgment of qualified healthcare professionals. All clinical decisions—especially those concerning patient care, procedural planning, or surgical interventions—must be made by board-certified and appropriately credentialed medical practitioners based on their own professional expertise, institutional protocols, and applicable regional regulations.
While every effort has been made to ensure the accuracy, currency, and relevance of the information presented, AVISTA makes no representations or warranties, express or implied, regarding the completeness, applicability, or clinical appropriateness of the content. We assume no responsibility or liability for any direct, indirect, incidental, or consequential harm, loss, or damage resulting from the use of any information or guidance provided herein.
AVISTA does not endorse any specific device, technology, or clinical approach mentioned unless explicitly stated, and any reference to commercial products or services is for educational illustration only. Readers are strongly encouraged to consult official guidelines, product IFUs, and institutional policies before implementing any technique or procedure discussed on this site.
Use of this website and its content constitutes agreement to these terms. For full legal terms, please refer to our Terms of Use and Privacy Policy.