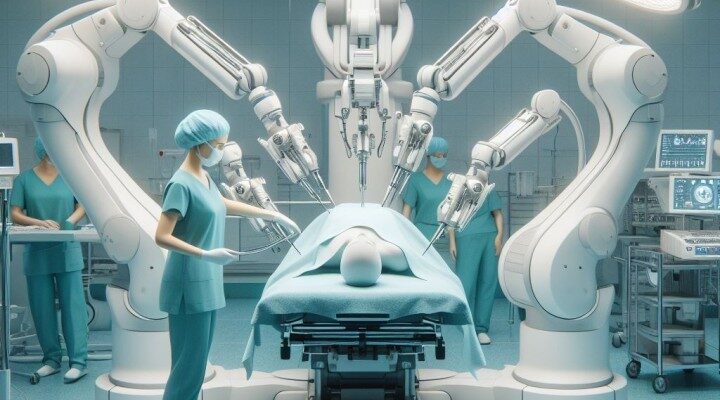
The adoption of surgical robotics in general abdominal and thoracic procedures is no longer a question of if, but how. For hospitals, the challenge lies in launching a program that delivers measurable clinical benefits while ensuring a clear and sustainable return on investment (ROI).
A successful robotics program is not built around a device: it is built around a system.
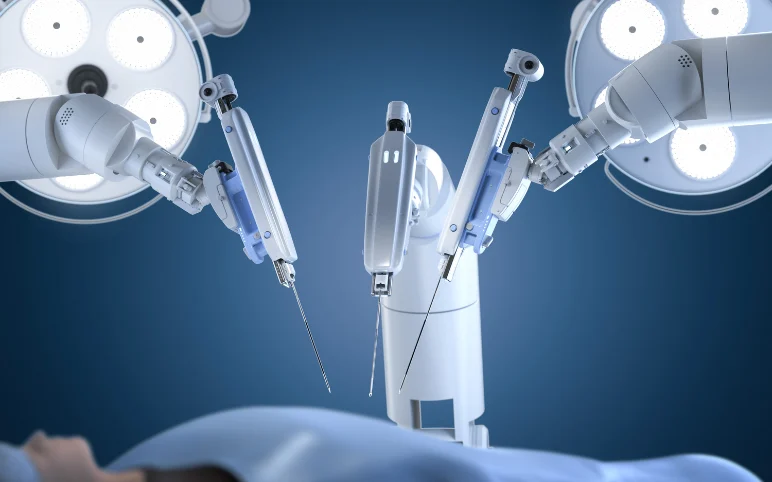
1. Start with Clinical Indication, Not Technology
One of the most common pitfalls in launching a robotic surgery program is allowing the technology to drive the strategy, rather than the clinical need. Institutions that succeed take the opposite approach—defining where robotics will add value before committing to the platform itself.
A strong foundation begins with a clear understanding of procedural demand, focusing on areas such as colorectal surgery, hernia repair, or thoracic resections where volumes are predictable and sustainable. It also requires identifying surgeons who are already experienced in minimally invasive techniques, as they are best positioned to transition effectively into robotic workflows. Most importantly, procedures should be selected based on where robotics offers a tangible advantage—whether through improved precision, better ergonomics, or enhanced access in complex anatomical spaces.
When implemented this way, robotics becomes a natural extension of an existing clinical pathway, strengthening and refining it, rather than attempting to build a new program around the technology alone.

2. Build the Right Team, Not Just the Surgeon
Strong outcomes in robotic surgery are rarely the result of individual skill alone; they reflect how well the entire team functions as a coordinated unit. The technology places new demands on workflow, communication, and intraoperative support, making consistency across the team just as important as surgical expertise.
At the core of a successful program is a surgeon with a solid foundation in minimally invasive techniques, supported by anesthesiology teams familiar with the physiological implications of prolonged procedures and patient positioning. Equally important are scrub nurses who are comfortable with robotic instrumentation and workflow, as well as biomedical engineers who ensure system readiness and can respond quickly to technical issues. In many settings, the involvement of an experienced clinical specialist further strengthens the team, providing procedural insight and real-time technical support during the early stages of adoption.
The consistency of the team directly correlates with complication rates and procedural efficiency.

3. Structured Training: From Simulation to Supervised Practice
A safe and effective launch of a robotic surgery program depends on a disciplined, stepwise training pathway. This typically begins with simulation-based learning, where surgeons develop familiarity with the console and instrument control in a risk-free environment. It then progresses to hands-on training through dry or wet labs, allowing teams to translate those skills into more realistic procedural settings. The transition into clinical practice is best supported by proctored cases under the guidance of experienced mentors, before gradually moving toward independent operating.
The true measure of training effectiveness is not simply the number of cases performed, but the time required to reach consistent procedural proficiency. Institutions that overlook this structured approach often encounter avoidable challenges—prolonged operative times, higher complication rates, and a lack of confidence among surgeons and operating teams.
4. Standardization of Workflow and Equipment
In robotic surgery, efficiency is rarely a function of speed alone—it is a function of consistency. Programs that achieve reliable performance do so by standardizing every aspect of the procedural workflow, from port placement strategies tailored to each operation, to predefined instrument sets and setup protocols. Even seemingly minor elements, such as docking sequences and troubleshooting pathways, benefit from being clearly defined and consistently executed.
This level of standardization creates a predictable operating environment, reducing variability between cases and minimizing dependence on individual staff experience. Over time, it translates into shorter, more consistent operative durations, fewer intraoperative disruptions, and a smoother integration of the robotic system into routine surgical practice.

5. Defining ROI beyond the capital cost
The financial performance of a surgical robotics program cannot be assessed solely on the initial capital investment. In practice, its value becomes evident through a combination of operational efficiency, clinical outcomes, and institutional positioning. On the direct side, programs that are well-structured tend to see a steady increase in case volumes, fewer conversions to open surgery, and a measurable reduction in length of stay and ICU utilization—each contributing to more efficient resource use and improved patient throughput.
Equally important, however, are the indirect drivers of value. A well-executed robotics program enhances the hospital’s reputation, attracting both patients seeking advanced care and high-caliber surgeons looking for a technologically progressive environment. Over time, it also enables the expansion into more complex procedures that may not have been feasible otherwise.
Ultimately, return on investment in surgical robotics is not a function of pricing strategy. It is the result of disciplined implementation, consistent utilization, and the ability to integrate the technology into a high-functioning clinical and operational ecosystem.
6. Volume Strategy: The Key to Sustainability
The long-term viability of a surgical robotics program is ultimately determined by utilization. Regardless of the sophistication of the technology, underused systems quickly become a financial and operational burden. Successful programs approach this proactively, building volume through procedures that are both high in demand and technically reproducible, allowing teams to develop consistency and confidence early on.
As experience grows, the program can expand into more complex indications, where the true clinical advantages of robotics become more evident. This gradual progression is critical—not only for maintaining patient safety, but also for ensuring that efficiency improves in parallel with case complexity.
In practical terms, sustainable programs typically evolve toward a steady throughput of multiple cases per day on each system within the first year to eighteen months. Institutions that fail to reach this level of utilization often struggle to justify the investment, making low case volume one of the most common—and most avoidable—reasons for program stagnation or failure.
7. Risk Management and Patient Safety
The early phase of any robotic surgery program is inherently vulnerable. Without the right controls in place, variability in technique, unfamiliar workflows, and overambitious case selection can quickly translate into avoidable complications. Programs that succeed recognize this upfront and deliberately build a safety-first framework into their initial rollout.
This typically begins with disciplined patient selection, favoring straightforward cases that allow the team to develop technical confidence without unnecessary risk. At the same time, the presence of experienced proctors during the initial cases provides not only technical oversight, but also a structured learning environment that accelerates safe skill acquisition. Equally important is the continuous monitoring of outcomes—tracking complication rates, procedural efficiency, and early signals of deviation—so that adjustments can be made in real time rather than retrospectively.
A critical, and often overlooked, component of this framework is the establishment of clear conversion protocols. The decision to convert to an open or conventional minimally invasive approach should never be delayed or perceived as a setback. On the contrary, the willingness to make that decision at the right moment reflects sound clinical judgment and program maturity. In the early stages especially, safety is not defined by completing every case robotically, but by consistently making the right decision for the patient.

8. Data-Driven Program Optimization
High-performing robotic programs are not static—they evolve continuously, guided by objective data rather than assumptions. From the outset, it is essential to establish a structured system for tracking key performance indicators, including operative times, complication profiles, conversion rates, length of stay, and overall cost per case. These metrics provide a clear and unbiased view of how the program is functioning, both clinically and operationally.
When analyzed consistently, this data becomes a powerful tool for improvement. It allows teams to identify inefficiencies in workflow, refine procedural steps, and support surgeons as they progress along the learning curve. Over time, it also creates a credible foundation for strategic decisions—whether that involves expanding into new indications, increasing system utilization, or investing in additional platforms.
Ultimately, programs that embrace a data-driven approach are better positioned to deliver predictable outcomes, demonstrate value to stakeholders, and sustain long-term growth with confidence.

Final Thought: Robotics as a Long-Term Clinical Platform
The institutions that derive real value from surgical robotics are those that understand it is not simply a piece of equipment to be acquired, but a program to be built and sustained. Its impact unfolds over time, shaped by how effectively it is integrated into clinical practice, training, and operational workflows.
When approached with the right level of discipline and structure, robotics has the potential to enhance surgical precision, broaden the scope of treatable cases, and elevate the overall standard of care. More importantly, it positions healthcare facilities not just as adopters of technology, but as leaders in the evolution of modern surgical practice.